Have you ever wondered what an Apgar is? Or, just as accurately, WHO Apgar is?
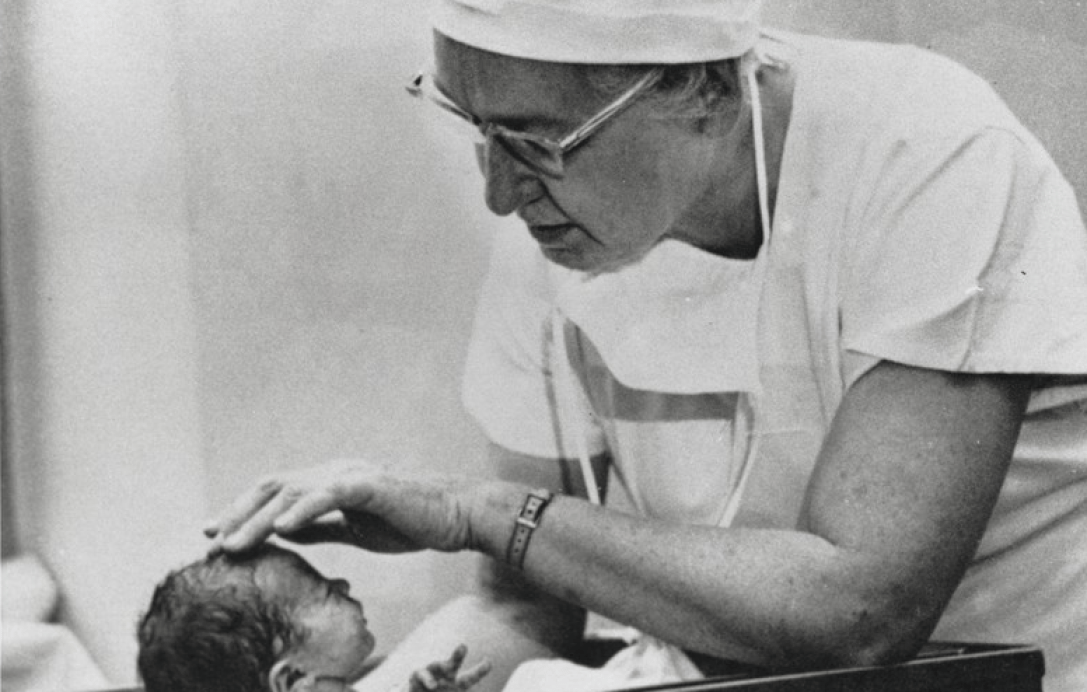
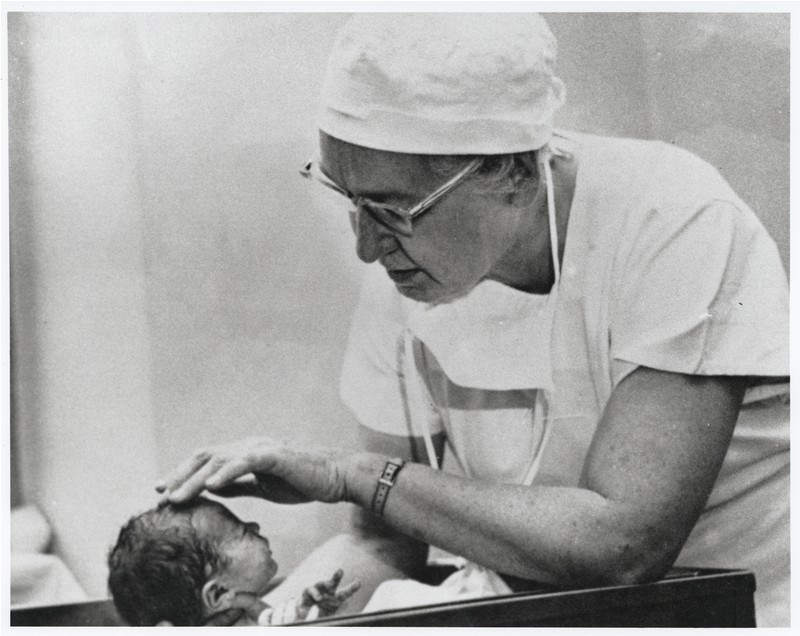
Well, in its first usage, “Apgar” was a name. Virginia Apgar was a doctor and scientist who was born in 1909 and passed away in 1974. During her lifetime, she made myriad contributions to fields including anesthesiology and teratology, studying how to make pain relief safer and what causes birth defects. Perhaps her most well-known contribution is the Apgar score.
The Apgar score is a way to quantify how well an infant is doing, physically, after birth.
The scale ranges from 0 to 10, with higher being better. It is comprised of five categories, each providing between 0 and 2 points. Here are the categories, followed by the three criteria that determine a score of 0, 1, and 2 respectively.
1) color (blue, pink in torso but blue in extremities, or pink all over)
2) heart rate (absent, under 100 beats per minute, over 100 beats per minute)
3) reflexes (no reaction to stimulation, a grimace, a cry or other strong reaction)
4) muscle tone (floppy, flexing, or active)
5) respiration (not breathing, breathing slowly or irregularly, breathing and crying normally).
Dr. Apgar developed this score in 1952 as a way to systematize a quick overview of how the baby is doing. It has become standard practice in the United States (ACOG – The American College of Obstetricians and Gynecologists –, for example, recommends the Apgar score as “an accepted and convenient method for reporting the status of the newborn infant immediately after birth and the response to resuscitation if needed”).
The Apgar score got its name from its creator, but “Apgar” is also a handy mnemonic:
1) activity (indicating muscle tone)
2) pulse (indicating heart rate)
3) grimace (indicating reflexes)
4) appearance (indicating color)
5) respiration (indicating, well, respiration. That one was easy to make work!).
OR
American Pediatric Gross Assessment Record.
Here’s how the scoring goes. Typically, a nurse, pediatrician, OBY/GYN, or midwife will do an assessment of the infant at 1 minute and 5 minutes after birth. Usually, infants will get a higher score at 5 minutes than they did at 1 minute, as their body adjusts to the outside world. If the infant’s score is low at 1 minute or at 5 minutes, providers will intervene to help the baby adjust.
I want to emphasize that it’s really rare for a newborn to score a 10 at either of these points, so any sense of grade inflation you might have or desire for perfectionism isn’t something that will be helpful in understanding what this means! For example, my daughter scored a 7 at her 1-minute and a 9 at her 5-minute, and she had a completely calm transition into the outside world with no complications. And, in fact, nearly all babies score low on the criteria of color, since blue extremities are very common after birth. So, it’s very important to remember that a healthy baby can easily receive a score less than 10.
A medical provider can explain to you what a particular infant’s Apgar score means. Also, since the Apgar score is usually just used for a quick overview of the infant’s health, if there is a medical difficulty, medical providers will use more specified tests to further detail baby’s condition.
So, TLDR: Apgar is a quick and easy way to assess an infant’s physical well-being, and an awesome scientist whose contributions have helped standardize indications that a newborn needs some help after birth.
If you’d like to learn more about Dr. Apgar, check out this biography or read her papers at the U.S. National Library of Medicine website.